Chewing muscles do more than chew. They position the mandible such that the most stable intercuspation can be reached with as straight a movement as possible. For instance, if the back teeth do not support the bite adequately, because they tilted into the gap of an extracted tooth or have been ground down, specific muscles will torque the mandible up in the posterior to bring those teeth closer to their antagonistic teeth so that they are brought into contact when biting. This torque will then compress the TMJ’s . However, it not only occurs when biting, but the resting position of the mandible is this changed, meaning that muscle tension and joint compression is maintained all of the time, even when you do not bite. This enables you to fit your teeth together at the blink of an eye without having to rearrange your mandibular posture first. Most of the time, people are completely unaware of such accommodations until they experience symptoms – which then often are misdiagnosed.
Every contact with teeth fires off sensory impulses from nerve endings in your periodontal ligaments telling the muscles how well they have succeeded in hitting your bite. This is a reflex process we are not conscious of and it controls mandibular posture and the necessary muscle tension to maintain it. It is like an automatic correction program that makes you able to live quite well in most cases, even if your bite is off – and it may be responsible for a lot of misunderstandings about the function of teeth in dentistry.
FreeBite therapy cushions are specifically shaped such that the first contact with them occurs on the posterior teeth, the very opposite of the problem many TMJ patients experience, whose front teeth touch first. Of course this contact is resilient and the bite cushion molds to the teeth until all side teeth are in contact. However, the reflex runs the other way around now, telling the muscles torquing the back of the mandible up to release and let go. Their tension is no longer required to achieve posterior tooth contact. The bite cushions of the FreeBite comfort have no wedge shape and do therefore not address joint compression as aggressively.
FreeBite therapy is started by lightly chewing or tapping the teeth on it for 5-15 minutes. Loosely moving the chewing muscles aids their micro circulation, providing muscle cells with fresh oxygen and pumping the lymph. The more chewing muscles recover, the easier and free they move. After a while they will have learned again how to relax..
Later, when you have become used to the FreeBite between your teeth, you do not have to chew it if you begin wearing it for longer time periods anymore. Your muscles will learn how to quickly switch from working with your existing bite and working with your FreeBite.
Yes. Everybody can compare how wide the mouth opens before and after using the FreeBite. Equally, you can assess how well you can move your mandible from side to side or if there is discomfort or joint noise during movement. You can also look in the mirror to compare how well you can turn your head from side to side before and after you use your FreeBite. Your therapist may assess changes elsewhere in your body and in this way find out which problems are caused by your bite. If using the FreeBite brings about no change in your symptoms, they probably are not related to your bite. This also can provide important information for problems such as headaches or tinnitus which can have a lot of unrelated causes. If your bite is not the problem, nobody should try to change it, possibly making it an additional one! Rather, one should look for other possible causes of your symptoms.
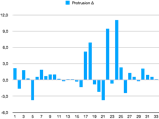
But the effect of the FreeBite on muscle tension can also be measured directly and objectively. Electromyography is a fairly complex technology, but it can bring the tiny electrical potentials to light which operate in your muscles. In the picture you see resting potentials of 4 chewing muscles (masseter and temporalis, left and right) and 4 cervical muscles (trapezius and sterno-cleido-mastoid, left and right). Each blue column represents a 15 second averaged sample, the left one before and the right one after using a FreeBite.
You can see the improved relaxation in the lower right columns after lightly chewing a FreeBite air medium for 12 minutes, up to 76% less residual muscle tension! Interestingly, three of the four neck muscles responded favorably as well to the FreeBite-chewing. This is a sign for a descending adaptive chain reaction where not only chewing muscles are involved in mandibular accommodation, but cervical muscles as well.
Mandibular mobility also can be objectively measured, in this case using a mandibular kinesiograph (Myotroncis, Inc.). 33 patients were compared in the order of their appointments for assessment in a dental practice specialized in TMJ. Their mandibular mobility was recorded before and after chewing on a FreeBite therapy cushion for 15-25 minutes. The second measurement was taken with the FreeBite still between the teeth, so that they could not reach tooth contact by 8 mm on average.
Since chewing on a FreeBite may correct the mandibular posture, the starting point for comparative measurements of mandibular mobility in the horizontal plane may have shifted. This is the reason why the second measurement was taken with the FreeBite still between the teeth, as those measurements were not originally taken to assess the effectiveness of the FreeBite, but in order to uncover a shift in mandibular posture. Lateral mobility can still be compared by simply adding the amount of movement to the right to that to the left, thus obtaining a sum total regardless of the starting point. The measurement does not represent any forced manipulation of the mandible, but pure voluntary movement as performed by the patients chewing muscles alone.
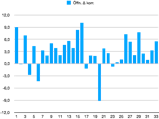
It might be reasonable to expect a decrease in lateral mobility when it is recorded with the teeth further apart due to the FreeBite. But this was only seen in 9 out of 33 cases (3 of which were negligibly small) while in 23 cases the lateral range of motion increased after chewing on a FreeBite therapy cushion in spite of the second measurement having been taken with the teeth further apart than the first. In 5 cases the increase was greater than 4 mm, suggesting the resolution of a blockage in one or two TMJ’s to displaced disks having repositioned.
The extent of mandibular protrusive range could also be expected to decrease the further apart the teeth are during measurement. In addition, a decrease of the protrusive mandibular movement might be expected in all those cases where the mandibular posture initially was displaced to the posterior and chewing on a FreeBite resulted in a more anterior starting position for this movement. But here as well an increase was observed in most cases instead. A decrease was found in 11 of 33 cases, four of those insignificantly small. In 22 cases an increase of protrusive mandibular mobility resulted, in 4 cases by more than 4 mm, suggesting the resolution of a previously anteriorly displaced articular disk.
Mouth opening increased in 27 of 33 cases where case No. 20 was an exception. He had sustained multiple cervical injuries during paragliding and bungee jumps. After the first measurement of his maximal mouth opening he developed a neck ache which was not resolved by chewing on a FreeBite therapy cushion for 20 minutes. His motivation to cooperate during the second measurement was compromised by his neck ache and 20 minutes also may well have been too long for his initial FreeBite therapy session.
This demonstrates the need for a word of caution: While the stimulation provided by the FreeBite leads to positive results in the vast majority of the cases, it can be too strong for some, especially if it is initially overdone. This is the reason for the development of the FreeBite comfort with flat bite cushions without shape. While the therapeutic effect may be slower to unfold, it provides a more gentle treatment alternative to FreeBite therapy cushions.
Except for case No. 20, mouth opening was reduced only in 5 out of 33 cases and only in two of those to any significant extent. On the other hand, 12 cases experienced significantly improved mouth opening which they also felt subjectively. These recorded measurements were corrected by the average distance by which the FreeBite blocks tooth contact and demonstrate the effect of a single FreeBite therapy session lasting on average 20 minutes. Further studies would be of interest, for instance investigating the effects of daily use of FreeBites after a week or two!